Herniated Disc
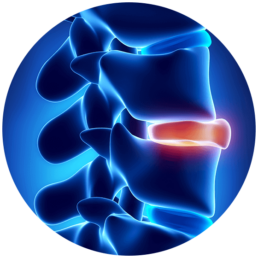
Herniated Disc Symptoms & Treatment Options
Separating our vertebrae are tiny, gel-filled cushions known as intervertebral discs. Intervertebral discs function to connect our spinal vertebrae and provide impact absorption between the adjacent bones of our spine. A herniated disc occurs when the exterior casing of this protective disc breaks open or cracks, releasing its jelly-like interior into the spinal canal. A ruptured disc often collapses upon itself, pinching nearby nerves and diminishing the spine’s ability to absorb compressive forces.
When we are young, our intervertebral discs are resilient and rubbery. However, as we age, our discs deflate from the ever-increasing impact of everyday wear and tear. As our discs degenerate, they undergo adverse changes. They lose their elasticity, suffer dehydration, and become more prone to disc herniation. An unexpected injury, such as a car accident, can cause these changes to occur instantaneously—instead of over the course of decades.
In addition, our vertebrae contain built-in passages that allow our nerves to fan out from the spinal cord to other regions of our body. These nerves dictate movement, sensation, and our awareness of pain. When these openings become obstructed because of herniated disc material, our spinal nerves often become pinched. Nerve impingement not only generates a great deal of pain, but can also lead to loss of sensation and motor control in our extremities.
Fortunately, herniated or slipped discs are highly treatable. At the Advanced Spine Center, our team of herniated disc experts uses innovative, minimally invasive, and individualized treatment plans to secure relief for thousands of patients with ruptured discs each year.
Regardless of the location of your injury, however, common warning signs of disc herniation include:
Pain that increases with the movement of your limbs
Pain that increases with the extension and compression of your back
Muscular weakness or inflammation near the site of disc herniation
An aching, burning, or tingling sensation in the muscles or limbs
Walking even a short distance aggravates your pain
Discomfort that worsens exponentially when engaging in strenuous activity
Pain that shoots into the arms (radiculopathy) or legs (sciatica)
Symptoms of a Herniated Disc
The symptoms of a herniated disc can range from unnoticeable to severe. Some people never even notice that they have a herniated disc, whereas others experience debilitating pain or limited mobility. When symptoms are present, the location of the disc rupture often determines how symptoms appear. Herniated discs are most common in the lumbar spine (or lower back), because this region of the torso bears the brunt of the upper body’s weight. However, disc herniation can also occur in the cervical (neck) region—or less commonly—in the thoracic (mid-back) segment of the spine.
Worried that your symptoms might suggest the presence of a herniated disc? At the Advanced Spine Center, we believe that everyone deserves a comprehensive and considerate approach to spine health. Our award-winning Top Doctors include Patient’s Choice and Compassionate Doctor award recipients. Contact the Advanced Spine Center today at (973) 538-0900 to receive personalized care from one of our distinguished surgeons.
Diagnosing a Herniated Disc
Herniated discs are a fairly common condition, especially for patients who are 65 years of age or older.
Regardless of your age, however: When you start experiencing herniated disc symptoms, it’s important to see a doctor for a physical exam. The source of your pain will be determined, which will involve an examination of your muscular strength and nerve function. You may also be asked to move certain ways and the affected area will be palpated, or touched. Additionally, your doctor will take a medical history and may perform X-rays, MRI scans, CT scans, or discograms.
The appropriate treatment will be determined. This is important since the ultimate complication of a herniated disc is saddle anesthesia, which occurs when sensation is lost in the backs of the legs, the inner thighs, and around the rectum. While the symptoms can improve, there is also the chance that they will worsen. If you find that you can’t perform activities like you used to, it’s time to seek medical attention.